A man is yelling for help. He looks to be about 65, is unkempt and in a wheelchair that he can only roll backward with unsteady feet. I’ve seen him before on my street. Sometimes he says hello; other times he’s engaged with unseen entities. Today, he says that God has abandoned him, and he wants to die. He howls in pain and asks someone to call 911. I look around and realize that I am that someone, and I oblige, even as he ignores my pleas to stay put. There’s a fecal odor coming from the trash bag he carries, and flies circle relentlessly. I wonder, not for the first time, how a human being could reach such a state in an abundant society.
A firetruck arrives, and I watch from a distance as EMTs approach the man. He shakes his head, refusing their efforts. The EMTs get back into their engine, and the man disappears into the streets.
About a week later, I see him again — this time, cleaned up in a hospital gown. He’s clear-eyed as he explains that his caseworker got him to the hospital, where he was given a proper meal and scheduled for surgery. “You have a caseworker?” I ask, but his lucidity is fleeting.
I see him a few more times, in varying states of filth and clarity, then never again.
For those who live in Sacramento or most any urban center in America, this story may ring familiar. For those who don’t, the apparent ease with which city dwellers walk past someone exhibiting psychosis may seem like apathy. But many will tell you it’s a learned helplessness instilled by decades of live-and-let-live policies concerning mental health and substance use.
Related: The Crusading Doctor: Sacramento-based WellSpace Health thrives with a unique approach to homeless and mentally ill patients
In recent years, however, leaders have changed their tune, responding to a growing sentiment that intervention may sometimes supersede autonomy when it comes to humane outcomes for people with mental illness and their communities.
Recent legislation signals that the priority is getting people into treatment, but whether that translates to large-scale impact is less clear.
How we got here
In the mid-20th century, public opinion was turning against psychiatric hospitalization as the standard of care. Concerns about horrendous conditions inside state-run hospitals had entered the national zeitgeist, fueled by reports of patients with very few legal rights living in abject filth and suffering inhumane treatments. Outrage coincided with the advent of antipsychotic drugs, leading to deinstitutionalization in favor of community treatment centers.
At least, that was the vision. Pres. John F. Kennedy promised a robust system of community treatment centers, but following his death in 1963, only about half were built, and funding was insufficient.
Yet deinstitutionalization continued. In 1967, Gov. Ronald Reagan signed the Lanterman-Petris-Short Act, which placed strict limits on involuntary commitment and effectively emptied the state’s mental hospitals. Among its provisions is the 5150 hold, which permits involuntary placement in a psychiatric facility for up to 72 hours while the detainee is assessed for further treatment. To be detained, an individual must be deemed a danger to themself or others or “gravely disabled,” a designation that carries a heavy burden of proof.
Then-California Gov. Ronald Reagan with his family in 1967, the
year he signed the Lanterman-Petris-Short Act, which placed
strict limits on involuntary commitment and effectively emptied
the state’s mental hospitals. (Public domain photo)

The result is the world we inhabit now, one where streets and prisons serve as de facto psych wards. This reality became even more visible in 2011, when Gov. Jerry Brown signed legislation to reduce the state’s crowded prison population.
“Creatures of the law”
California’s current governor has one eye on the 2028 presidential election, and a triad of the state’s most visible crises — mental health, drug use and homelessness — is a pressure point.
As the nation’s most populous state, California has more unhoused people than any other: A 2024 point-in-time count found 187,084 individuals. Within that population, 27 percent said they’d been hospitalized due to a mental health condition, and 65 percent reported a history of using amphetamines, cocaine or non-prescribed opioids regularly, according to a 2023 survey conducted by UC San Francisco.
An encampment in Oakland. (Shutterstock photo)

In the first year of his second term, Gov. Gavin Newsom signed Senate Bill 43, which broadens the criteria for “gravely disabled,” adding severe substance use disorder as a qualifying condition alongside mental illness and chronic alcoholism.
While it’s a meaningful change, it hasn’t significantly altered the landscape in Sacramento.
Initially, there was trepidation that SB 43 would overwhelm emergency rooms, but that hasn’t been the case, according to Sacramento County Behavioral Health Director Ryan Quist. That’s because law enforcement officers often can’t tell the difference between a mental health crisis and substance-induced psychosis, taking drug cases to the ER before jail. “We were already seeing the full volume of folks at the emergency departments prior to the law changing,” he says.
Nor has there been an influx of individuals deemed gravely disabled, because substance use disorders and mental illness are often co-occurring.
Related: The Capital Region Is in the Vanguard of Autism Research and Treatment
But there’s another new law that’s wielding more weight. In 2022, Newsom signed the CARE Act — a significant step toward the community-based treatment system that deinstitutionalization promised but never delivered.
An acronym for Community Assistance, Recovery and Empowerment, the CARE Act establishes a civil court process, known as CARE Court, through which people diagnosed with a qualifying psychotic disorder can access wraparound treatment and support services. What makes CARE Court distinctive is that referrals can come from virtually anyone — a family member, first responder or roommate — not just a doctor.
The law has been criticized by some, including Disability Rights California, for potential discrimination and civil rights concerns. Judges can impose a court-ordered “CARE plan” if an individual refuses treatment, but that outcome is rare, according to a 2025 report from CalMatters, and some counties have forgone CARE plans altogether. In Sacramento County, the program is “strictly voluntary.”
CARE Court treads more softly than originally proposed. The initial legislative draft included substance use as a qualifying disorder. Additional amendments further narrowed eligibility, increased the burden on petitioners, prioritized voluntary treatment over court-ordered plans and gave counties the freedom not to provide certain services.
Related: Perspective: The Ever-Growing Sacramento Homeless Crisis
Statewide, enrollment numbers are lower than projected. All counties were required to implement CARE Court starting in December 2024, and rollout has been slow. As of July 2025, just 2,421 petitions had been filed statewide, and only 528 had resulted in treatment agreements or plans, according to a CalMatters survey.
Whether the law oversteps or doesn’t do enough is a matter of perspective, says Sacramento County Superior Court Judge Lawrence Brown, who presided over CARE Court in its first year. “We’re just creatures of the law. We will use the tools that have been provided. If the tools are expanded, we’ll use those tools as well.”
Sacramento County Superior Court Judge Jennifer K. Rockwell
presides over the county’s first CARE Court graduation ceremony
March 17, with graduate Lorenzo Leon and supporters in
attendance. (Photo courtesy of Sacramento County)

According to Quist, 144 CARE Court petitions had been filed in Sacramento County as of March 1. No data was provided on how many have resulted in treatment. The biggest challenges have been the paperwork for petitioners and securing more permanent housing for those who complete the program. “The central issue is that we don’t have affordable housing for those that need it,” Quist says.
Even so, Sacramento County outperforms those of a similar size on homelessness and behavioral health metrics. The unsheltered population is down by over 40 percent since 2023, according to a state dashboard, while more than 2,500 people are in full-service partnerships that provide 24/7 support for those with severe mental illness. The county has also been adding beds to its psychiatric care facilities, according to Quist.
“No way to live”
Alicia Leon used to go long stretches without seeing her adult son. One of the challenges of having a loved one with a psychotic disorder is that they may be unaware of their condition and distrustful of those who try to help. Alicia’s son, Lorenzo, was living on the streets when her petition for CARE Court was granted last year.
Lorenzo Leon enjoys a slice of cake at his graduation ceremony
and holds graduation presents with his mother, Alicia. (Photo
courtesy of Sacramento County)

According to Brown, CARE Court has changed the system by allowing anyone to petition a judge directly. “This is, to me, unprecedented to have a family member come directly and say, ‘We need help,’” he says.
For Lorenzo, help was given. During his year in CARE Court, he received psychiatric treatment and social services through a dedicated team, checking in with the court each month. CARE Court recipients are also provided with housing options, if needed. But first, they must be located and accept care.
Edward Pochay, a behavioral health peer specialist for Sacramento County, spends a lot of time playing detective — tracking down CARE Court recipients and introducing them to the program. He reads up on their history and tries to understand their perspective before making contact. In Lorenzo’s case, it was a matter of identifying the places he frequented and knowing his preferred nickname. “I would see him standing there and greet him by that name, which brought a secret smile to his face. So I knew we were on the right track,” Pochay says.
Lorenzo ultimately agreed to participate. When he left home, his care team would find him and persuade him to come back. Pochay says the lived experience of peer specialists like him makes them uniquely able to establish rapport with people struggling with mental illness, homelessness or substance use.
“A seed was planted. That person now knows there are people out there willing to go to great lengths to offer services without any negative encounter, that she can say no without consequences.”
— Edward Pochay, behavioral health peer specialist, Sacramento County
But they aren’t always successful. He describes a case where a woman living in an encampment littered with used syringes refused all help. “I can be disappointed. I can be let down. But frustration doesn’t factor in, because I cannot imagine what they are experiencing,” Pochay explains. “A seed was planted. That person now knows there are people out there willing to go to great lengths to offer services without any negative encounter, that she can say no without consequences.”
Pochay believes voluntary participation is integral to recovery, even if it takes many attempts before someone accepts help. He recalls a recipient referred by law enforcement who was “primed against the system” but ultimately won over through persistent contact. At a recent CARE Court appearance, he brought Judge Brown a gift and asked him for a hug. “You could feel the silence in the room for a moment. And then Judge Brown got up from his bench, came around to the podium … and gave him a hug,” Pochay says. “That’s what it’s about.”
On March 17, Lorenzo Leon became Sacramento County’s first-ever CARE Court graduate. His mother and care team were present at the courthouse to celebrate and share his cake. “Being on the street is no way to live,” Lorenzo said in a county press release. “So, you know, I did what I have to do, straightened up so now I have a place to live.”
For Pochay, true progress is measured in these moments. Another milestone, he says, was when Lorenzo’s mother started swimming in the mornings. “That just fills my heart. She was consistently seeing improvement in him to the point where she felt it was her time to do something for herself.”
If you or someone you know is experiencing a mental health
crisis,
call the 988 Suicide & Crisis Lifeline.
–
Stay up to date on business in the Capital Region: Subscribe to the Comstock’s newsletter today.
Recommended For You

Research Suggests That This Strong Emotion Can Be Harnessed to Improve Mental Health
How UC Davis scientists and educators recommend harnessing awe in the everyday
When was the last time you felt awe? You may call it something
else, but you know the sensation — the wide-eyed, hushed-voice,
goosebumps-down-the-back feeling that comes with grand, novel
experiences.
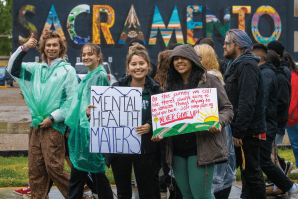
A Push for School-Based Mental Health
Ratcheted up by the pandemic, students’ mental health has become an important focus in schools
Schools and universities in the Capital Region have taken an array of approaches to assure mental health is one of the many pillars a student’s education addresses.

The Crusading Doctor
Sacramento-based WellSpace Health thrives with a unique approach to homeless and mentally ill patients
The homelessness crisis has seemingly coincided with a lack of sufficient behavioral health resources. Organizations like WellSpace could be well-positioned to take on a growing share of this vital work.

Status Check: WellSpace Moves Ahead on Behavioral Health
WellSpace Health gains Gold Seal for its Certified Community Behavioral Health Clinic
WellSpace is strengthening its behavioral work, announcing on Oct. 9 that its certified community behavioral health clinic had received the Gold Seal of Approval from The Joint Commission.




